Kara Kucinski |
Over the last 2 weeks, how often have you been bothered by the following problems?
Not at all
Several days
More than half the days
Nearly every day
Feeling nervous, anxious, or on edge
0
1
2
3
Not being able to stop or control worrying
0
1
2
3
Worrying too much about different things
0
1
2
3
Trouble relaxing
0
1
2
3
Being so restless that it is hard to sit still
0
1
2
3
Becoming easily annoyed or irritated
0
1
2
3
Feeling afraid as if something awful might happen
0
1
2
3
Column totals
_______
+ _______
+ _______
+ _______ =
Total score
_______
If you checked any problems, how difficult have they made it for you to do your work, take care of things at home, or get along with other people?
Not difficult at all
Somewhat difficult
Very difficult
Extremely difficult
This is calculated by assigning scores of 0, 1, 2, and 3 to the response categories, respectively, of “not at all,” “several days,” “more than half the days,” and “nearly every day.” GAD-7 total score for the seven items ranges from 0 to 21.
0–4: minimal anxiety
5–9: mild anxiety
10–14: moderate anxiety
15–21: severe anxiety
No Comments |
Kara Kucinski |
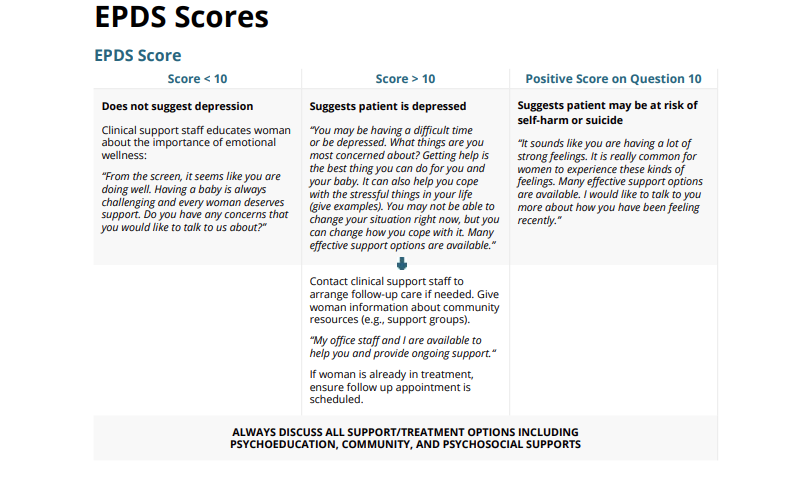
Score < 10
Score > 10
Positive Score on Question 10
Does not suggest depression
Clinical support staff educates woman about the importance of emotional wellness:
“From the screen, it seems like you are doing well. Having a baby is always challenging and every woman deserves support. Do you have any concerns that you would like to talk to us about?”
Suggests patient is depressed
“You may be having a difficult time or be depressed. What things are you most concerned about? Getting help is the best thing you can do for you and your baby. It can also help you cope with the stressful things in your life (give examples). You may not be able to change your situation right now, but you can change how you cope with it. Many effective support options are available.”
Suggests patient may be at risk of self-harm or suicide
“It sounds like you are having a lot of strong feelings. It is really common for women to experience these kinds of feelings. Many effective support options are available. I would like to talk to you more about how you have been feeling recently.”
Contact clinical support staff to arrange follow-up care if needed. Give woman information about community resources (e.g., support groups).
“My office staff and I are available to help you and provide ongoing support.”
If woman is already in treatment, ensure follow up appointment is scheduled.
ALWAYS DISCUSS ALL SUPPORT/TREATMENT OPTIONS INCLUDING PSYCHOEDUCATION, COMMUNITY, AND PSYCHOSOCIAL SUPPORTS
This resource has been adapted with permission from the MCPAP for Moms Pediatric Toolkit for Postpartum Depression.
No Comments |
Kara Kucinski |
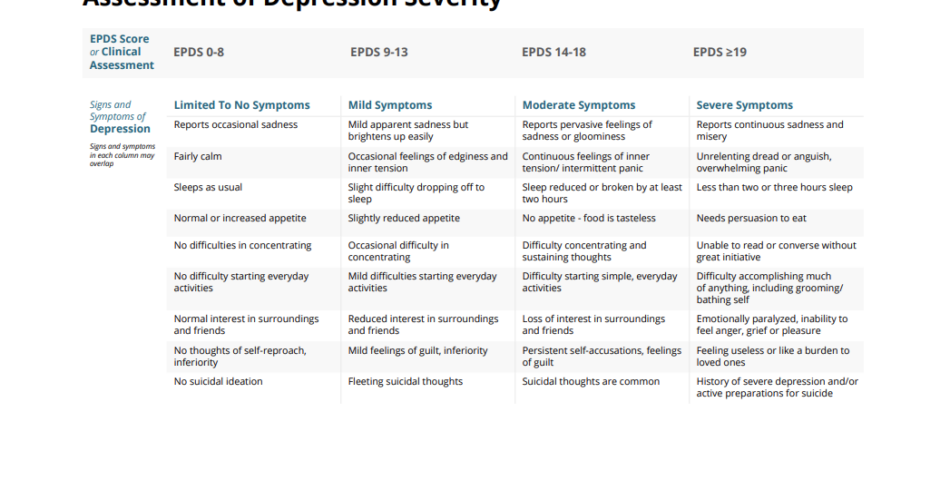
EPDS Score or Clinical Assessment
EPDS 0-8
EPDS 9-13
EPDS 14-18
EPDS ≥19
Signs and symptoms of Depression
Signs and symptoms in each column may overlap
Limited to no symptoms
Mild symptoms
Moderate symptoms
Severe symptoms
Reports occasional sadness
Mild apparent sadness but brightens up easily
Reports pervasive feelings of sadness or gloominess
Reports continuous sadness and misery
Fairly calm
Occasional feelings of edginess and inner tension
Continuous feelings of inner tension/intermittent panic
Unrelenting dread or anguish, overwhelming panic
Sleeps as usual
Slight difficulty drifting off to sleep
Sleep reduced or broken by at least two hours
Less than two or three hours of sleep
Normal or increased appetite
Slightly reduced appetite
No appetite – food is tasteless
Needs persuasion to eat
No difficulties in concentrating
Occasional difficulty in concentrating
Difficulty concentrating and sustaining thoughts
Unable to read or converse without great initiative
No difficulty starting everyday activities
Mild difficulties starting everyday activities
Difficulty starting simple, everyday activities
Difficulty accomplishing much of anything, including grooming/bathing self
Normal interest in surroundings and friends
Reduced interest in surroundings and friends
Loss of interest in surroundings and friends
Emotionally paralyzed, inability to feel anger, grief, or pleasure
No thoughts of self-reproach, inferiority
Mild feelings of guilt, inferiority
Persistent self-accusations, feelings of guilt
Feeling useless or like a burden to loved ones
No suicidal ideation
Fleeting suicidal thoughts
Suicidal thoughts are common
History of severe depression and/or active preparations for suicide
This resource has been adapted with permission from the MCPAP for Moms Pediatric Toolkit for Postpartum Depression.
No Comments |
Kara Kucinski |

(Discussion should include yet not be limited to the below)
If lactating: SSRIs and some other antidepressants are considered a reasonable treatment option during breastfeeding. The benefits of breastfeeding while taking antidepressants generally outweigh the risks. The amount of medication that goes into the breast milk is relatively small and there is no evidence of significant short or long term consequences to babies who are exposed to SSRIs through breast milk.
See Antidepressant Treatment Algorithm for guidelines on prescribing medications.
No Comments |
Kara Kucinski |
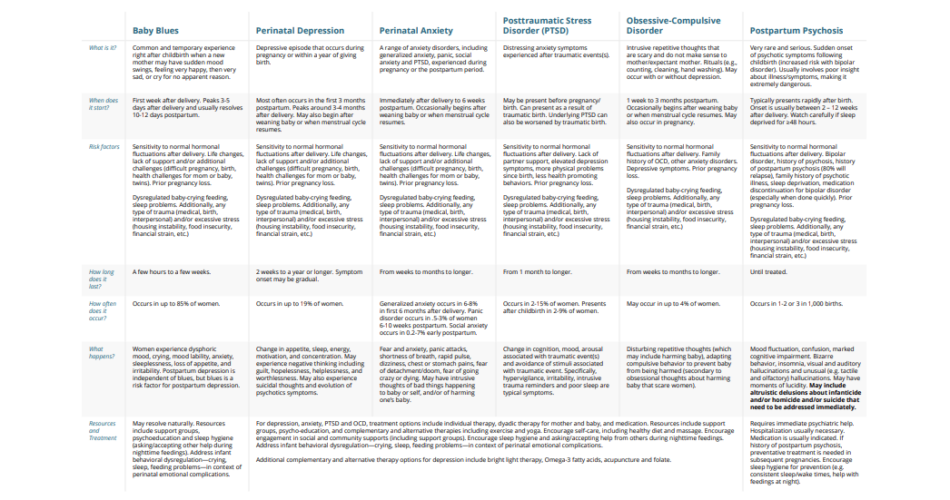
Baby Blues
Perinatal Depression
Perinatal Anxiety
Posttraumatic Stress Disorder (PTSD)
Obsessive-Compulsive Disorder
Postpartum Psychosis
What is it?
Common and temporary experience right after childbirth when a new mother may have sudden mood swings, feeling very happy, then very sad, or cry for no apparent reason.
Depressive episode that occurs during pregnancy or within a year of giving birth.
A range of anxiety disorders, including generalized anxiety, panic, social anxiety and PTSD, experienced during pregnancy or the postpartum period.
Distressing anxiety symptoms experienced after traumatic events(s).
Intrusive repetitive thoughts that are scary and do not make sense to mother/expectant mother. Rituals (e.g., counting, cleaning, hand washing). May occur with or without depression.
Very rare and serious. Sudden onset of psychotic symptoms following childbirth (increased risk with bipolar disorder). Usually involves poor insight about illness/symptoms, making it extremely dangerous.
When does it start?
First week after delivery. Peaks 3-5 days after delivery and usually resolves 10-12 days postpartum.
Most often occurs in the first 3 months postpartum. Peaks around 3-4 months after delivery. May also begin after weaning baby or when menstrual cycle resumes.
Immediately after delivery to 6 weeks postpartum. Occasionally begins after weaning baby or when menstrual cycle resumes.
May be present before pregnancy/ birth. Can present as a result of traumatic birth. Underlying PTSD can also be worsened by traumatic birth.
1 week to 3 months postpartum. Occasionally begins after weaning baby or when menstrual cycle resumes. May also occur in pregnancy.
Typically presents rapidly after birth. Onset is usually between 2 – 12 weeks after delivery. Watch carefully if sleep deprived for ≥48 hours.
Risk factors
Sensitivity to normal hormonal fluctuations after delivery. Life changes, lack of support and/or additional challenges (difficult pregnancy, birth, health challenges for mom or baby, twins). Prior pregnancy loss. Dysregulated baby-crying feeding, sleep problems. Additionally, any type of trauma (medical, birth, interpersonal) and/or excessive stress (housing instability, food insecurity, financial strain, etc.)
Sensitivity to normal hormonal fluctuations after delivery. Life changes, lack of support and/or additional challenges (difficult pregnancy, birth, health challenges for mom or baby, twins). Prior pregnancy loss. Dysregulated baby-crying feeding, sleep problems. Additionally, any type of trauma (medical, birth, interpersonal) and/or excessive stress (housing instability, food insecurity, financial strain, etc.)
Sensitivity to normal hormonal fluctuations after delivery. Life changes, lack of support and/or additional challenges (difficult pregnancy, birth, health challenges for mom or baby, twins). Prior pregnancy loss. Dysregulated baby-crying feeding, sleep problems. Additionally, any type of trauma (medical, birth, interpersonal) and/or excessive stress (housing instability, food insecurity, financial strain, etc.)
Sensitivity to normal hormonal fluctuations after delivery. Lack of partner support, elevated depression symptoms, more physical problems since birth, less health promoting behaviors. Prior pregnancy loss. Dysregulated baby-crying feeding, sleep problems. Additionally, any type of trauma (medical, birth, interpersonal) and/or excessive stress (housing instability, food insecurity, financial strain, etc.)
Sensitivity to normal hormonal fluctuations after delivery. Family history of OCD, other anxiety disorders. Depressive symptoms. Prior pregnancy loss. Dysregulated baby-crying feeding, sleep problems. Additionally, any type of trauma (medical, birth, interpersonal) and/or excessive stress (housing instability, food insecurity, financial strain, etc.)
Sensitivity to normal hormonal fluctuations after delivery. Bipolar disorder, history of psychosis, history of postpartum psychosis (80% will relapse), family history of psychotic illness, sleep deprivation, medication discontinuation for bipolar disorder (especially when done quickly). Prior pregnancy loss. Dysregulated baby-crying feeding, sleep problems. Additionally, any type of trauma (medical, birth, interpersonal) and/or excessive stress (housing instability, food insecurity, financial strain, etc.)
How long does it last?
A few hours to a few weeks.
2 weeks to a year or longer. Symptom onset may be gradual.
From weeks to months to longer.
From 1 month to longer.
From weeks to months to longer.
Occurs in 1-2 or 3 in 1,000 births.
How often does it occur?
Occurs in up to 85% of women.
Occurs in up to 19% of women.
Generalized anxiety occurs in 6-8% in first 6 months after delivery. Panic disorder occurs in .5-3% of women 6-10 weeks postpartum. Social anxiety occurs in 0.2-7% early postpartum.
Occurs in 2-15% of women. Presents after childbirth in 2-9% of women.
May occur in up to 4% of women.
Occurs in 1-2 or 3 in 1,000 births.
What happens?
Women experience dysphoric mood, crying, mood lability, anxiety, sleeplessness, loss of appetite, and irritability. Postpartum depression is independent of blues, but blues is a risk factor for postpartum depression.
Change in appetite, sleep, energy, motivation, and concentration. May experience negative thinking including guilt, hopelessness, helplessness, and worthlessness. May also experience suicidal thoughts and evolution of psychotics symptoms.
Fear and anxiety, panic attacks, shortness of breath, rapid pulse, dizziness, chest or stomach pains, fear of detachment/doom, fear of going crazy or dying. May have intrusive thoughts of bad things happening to baby or self, and/or of harming one’s baby.
Change in cognition, mood, arousal associated with traumatic event(s) and avoidance of stimuli associated with traumatic event. Specifically, hypervigilance, irritability, intrusive trauma reminders and poor sleep are typical symptoms.
Disturbing repetitive thoughts (which may include harming baby), adapting compulsive behavior to prevent baby from being harmed (secondary to obsessional thoughts about harming baby that scare women).
Mood fluctuation, confusion, marked cognitive impairment. Bizarre behavior, insomnia, visual and auditory hallucinations and unusual (e.g. tactile and olfactory) hallucinations. May have moments of lucidity. May include altruistic delusions about infanticide and/or homicide and/or suicide that need to be addressed immediately.
Resources and Treatment
May resolve naturally. Resources include support groups, psychoeducation and sleep hygiene (asking/accepting other help during nighttime feedings). Address infant behavioral dysregulation—crying, sleep, feeding problems—in context of perinatal emotional complications.
For depression, anxiety, PTSD and OCD, treatment options include individual therapy, dyadic therapy for mother and baby, and medication. Resources include support groups, psycho-education, and complementary and alternative therapies including exercise and yoga. Encourage self-care, including healthy diet and massage. Encourage engagement in social and community supports (including support groups). Encourage sleep hygiene and asking/accepting help from others during nighttime feedings. Address infant behavioral dysregulation—crying, sleep, feeding problems—in context of perinatal emotional complications. Additional complementary and alternative therapy options for depression include bright light therapy, Omega-3 fatty acids, acupuncture and folate.
Requires immediate psychiatric help. Hospitalization usually necessary. Medication is usually indicated. If history of postpartum psychosis, preventative treatment is needed in subsequent pregnancies. Encourage sleep hygiene for prevention (e.g. consistent sleep/wake times, help with feedings at night).
This resource has been adapted with permission from the MCPAP for Moms Pediatric Toolkit for Postpartum Depression.
No Comments |
Kara Kucinski |
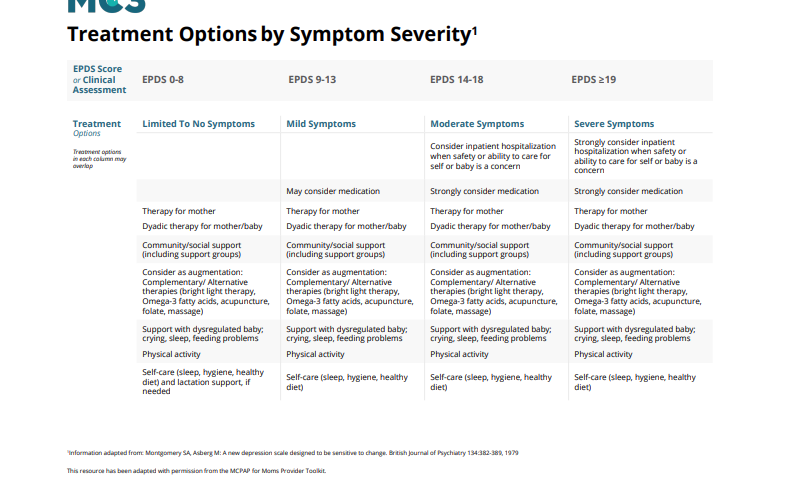
EPDS Score or Clinical Assessment
EPDS 0-8
EPDS 9-13
EPDS 14-18
EPDS ≥19
Treatment options
Treatment options in each column may overlap
Limited to no symptoms
Mild symptoms
Moderate symptoms
Severe symptoms
Consider inpatient hospitalization when safety or ability to care for self or baby is a concern
Strongly consider inpatient hospitalization when safety or ability to care for self or baby is a concern
May consider medication
Strongly consider medication
Strongly consider medication
Therapy for mother
Dyadic therapy for mother/baby
Therapy for mother
Dyadic therapy for mother/baby
Therapy for mother
Dyadic therapy for mother/baby
Therapy for mother
Dyadic therapy for mother/baby
Community/social support (including support groups)
Community/social support (including support groups)
Community/social support (including support groups)
Community/social support (including support groups)
Consider as augmentation: Complementary/ Alternative therapies (bright light therapy, Omega-3 fatty acids, acupuncture, folate, massage)
Consider as augmentation: Complementary/ Alternative therapies (bright light therapy, Omega-3 fatty acids, acupuncture, folate, massage)
Consider as augmentation: Complementary/ Alternative therapies (bright light therapy, Omega-3 fatty acids, acupuncture, folate, massage)
Consider as augmentation: Complementary/ Alternative therapies (bright light therapy, Omega-3 fatty acids, acupuncture, folate, massage)
Support with dysregulated baby; crying, sleep, feeding problems
Physical activity
Support with dysregulated baby; crying, sleep, feeding problems
Physical activity
Support with dysregulated baby; crying, sleep, feeding problems
Physical activity
Support with dysregulated baby; crying, sleep, feeding problems
Physical activity
Self-care (sleep, hygiene, healthy diet) and lactation support, if needed
Self-care (sleep, hygiene, healthy diet)
Self-care (sleep, hygiene, healthy diet)
Self-care (sleep, hygiene, healthy diet)
This resource has been adapted with permission from the MCPAP for Moms Pediatric Toolkit for Postpartum Depression.
No Comments |
Kara Kucinski |
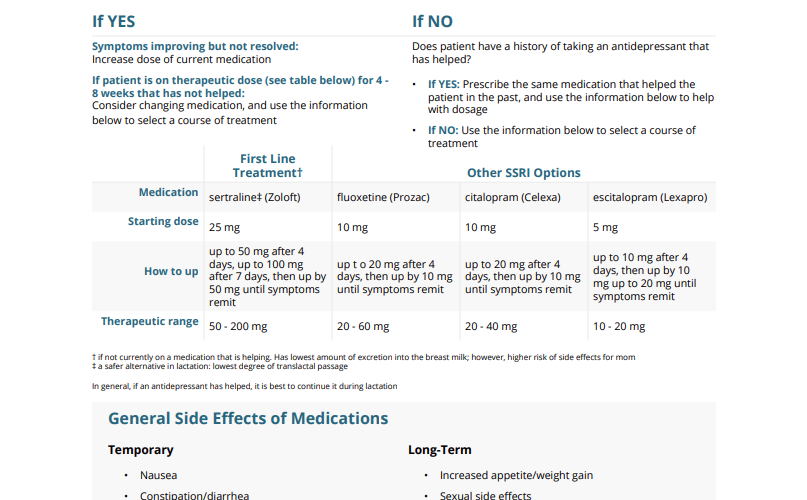
Symptoms improving but not resolved: Increase dose of current medication
If patient is on therapeutic dose (see table below) for 4 – 8 weeks that has not helped: Consider changing medication, and use the information below to select a course of treatment
Does patient have a history of taking an antidepressant that has helped?
• If YES: Prescribe the same medication that helped the patient in the past, and use the information below to help with dosage
• If NO: Use the information below to select a course of treatment
First Line Treatment
Other SSRI Options
Medication
sertraline (Zoloft)
fluoxetine (Prozac)
citalopram (Celexa)
escitalopram (Lexapro)
Starting dose
25 mg
10 mg
10 mg
5 mg
How to up
up to 50 mg after 4 days, up to 100 mg after 7 days, then up by 50 mg until symptoms remit
up to 20 mg after 4 days, then up by 10 mg until symptoms remit
up to 20 mg after 4 days, then up by 10 mg until symptoms remit
up to 10 mg after 4 days, then up by 10 mg up to 20 mg until symptoms remit
Therapeutic range
50 – 200 mg
20 – 60 mg
20 – 40 mg
10 – 20 mg
In general, if an antidepressant has helped, it is best to continue it during lactation
Temporary
Long-Term
Recommend patients take medication with food to decrease side effects Tell women only to increase dose if tolerating; otherwise wait until side effects dissipate before increasing For effects on fetus/neonate, see Discussing Antidepressant Use with Perinatal Patients.
2. Repeat EPDS in 2 – 4 weeks and re-evaluate depression treatment plan via clinical assessment
If no/minimal clinical improvement after 4-8 weeks
If clinical improvement and no/minimal side effects
If patient has no or minimal side effects, increase dose If patient has side effects that are severe/intolerable, or that do not resolve after 1-2 weeks, switch to a different medication
Reevaluate every month and at postpartum visit
This resource has been adapted with permission from the MCPAP for Moms Pediatric Toolkit for Postpartum Depression.
No Comments |
Kara Kucinski |

Patients with bipolar disorder are very sensitive to disturbances in sleep, and have a higher risk of postpartum psychosis than patients with depression or anxiety. Therefore, make sure to counsel them about the following:
No Comments |
Kara Kucinski |

Treatment of ADHD in the perinatal period is important to preserve overall functioning of the patient, as well as in some cases, to effectively control symptoms of disorders commonly comorbid with ADHD such as depression, anxiety, and substance abuse.
Please reference the algorithm below when caring for perinatal patients with ADHD:
Mild ADHD (Minimal Functional Impairment Off Medication)
Moderate ADHD (Some Functional Impairment Off Medication)
Severe ADHD (Significant Functional Impairment, Including Driving)
Optimize sufficient non-pharmacologic management strategies and ensure self-management strategies in place
Optimize non-pharmacologic strategies; consider when necessary use of stimulant
Maintain medication, consider closer obstetric monitoring for fetal growth and hypertensive disorders of pregnancy
No Comments |
Kara Kucinski |

The decision about whether to prescribe stimulants during the perinatal period should be made jointly with the patient after sharing information about the risks and benefits. For a good review article and demonstration of shared decision-making, please reference this article:
No Comments |